Vaccine recommendations
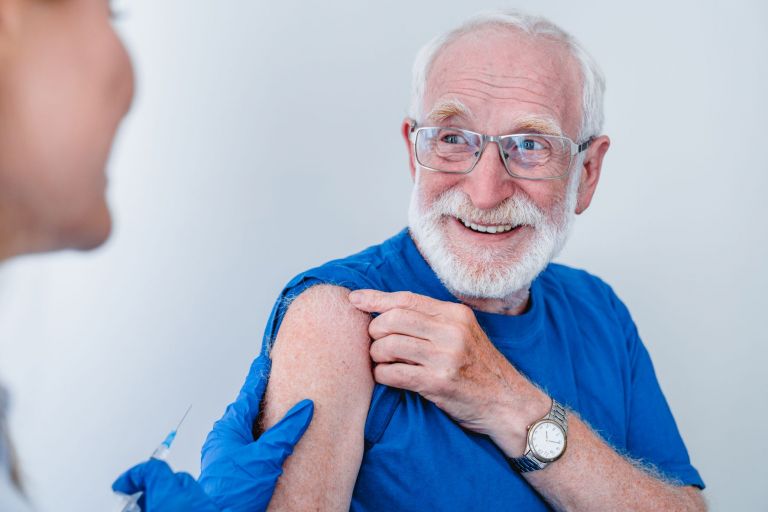
Get a COVID-19 vaccination
Find out if you are recommended to get your next COVID-19 vaccination.
COVID-19 vaccination for children
Vaccination is recommended for children aged 6 months and older at risk of severe COVID-19.
Get the facts about vaccination
Evidence-based answers to frequently asked questions about COVID-19 vaccines.
Proof of COVID-19 vaccinations
How to get proof of COVID-19 vaccination and download it to your mobile phone.
COVID-19 vaccines
The National Centre for Immunisation Research and Surveillance (NCIRS) provides information about different COVID-19 vaccines.
COVID-19 vaccination rates
Vaccination rates and related statistics, reported by the Australian Government.
People at higher risk of severe illness
Some groups of people – such as those aged 70 and over – are at higher risk of becoming very sick with COVID-19.
Talk to your doctor about vaccination and COVID-19 medicines like antivirals.

Easy Read and in-language resources
Contact us and find translation help
Contacts and enquiries
- Service NSW – information and advice for NSW residents and businesses. Phone 13 77 88
- Healthdirect – government-funded 24-hour health advice. Phone 1800 022 222
- Disability Gateway – information for people with disability. Phone 1800 643 787
Government services
- Mental health support, services and programs
- Service NSW Savings Finder – find rebates and vouchers relevant to you
- Business Concierge – tailored advice from Business Connect advisors. Phone 13 77 88
Language and interpreting support
- Translating and Interpreting Service (TIS National) – free service provided by the Australian Government. Phone 13 14 50
Last updated: